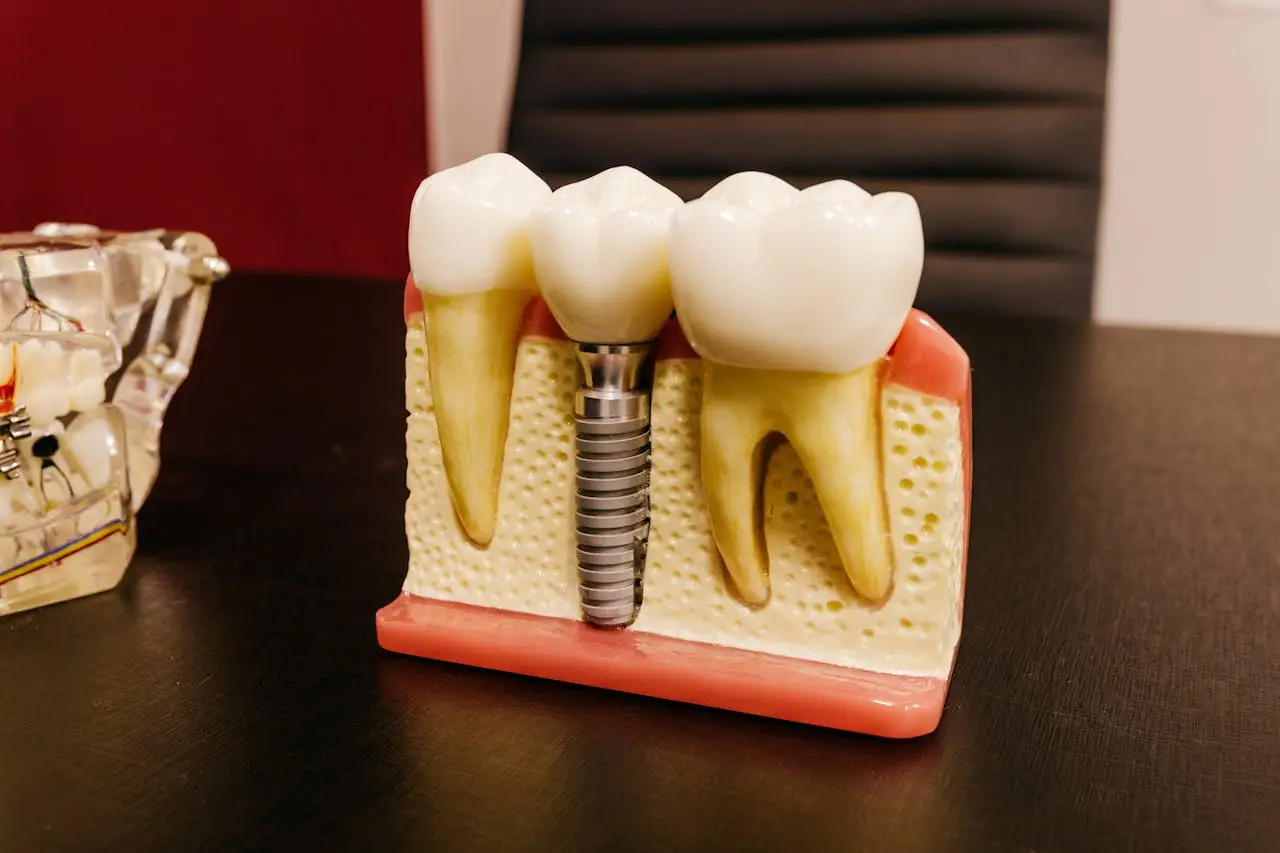
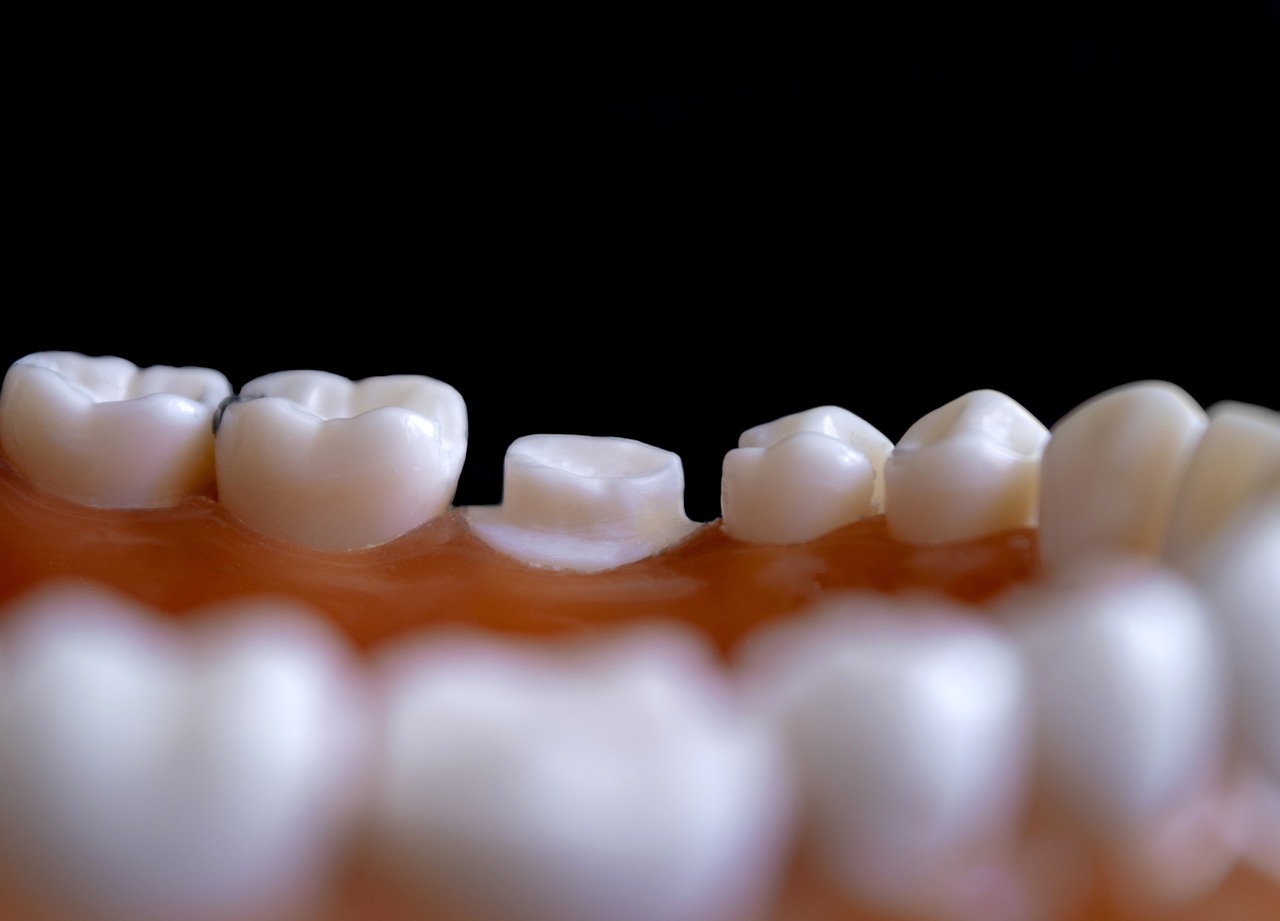
A good dental filling is increasingly seen as a lost art among many dentists due to a combination of factors such as time pressure, over-reliance on simplified techniques, reduced emphasis on craftsmanship, and evolving patient expectations for speed and aesthetics
Art and Science in Dental Fillings
Dental fillings require a blend of art and science—not just plugging a gap but restoring a tooth to its original shape, function, strength, and beauty. Many dentists focus on technical adequacy and speed rather than the fine details of form, marginal adaptation, and occlusion. This shift is partly due to increasing patient volume and economic pressures.
Causes for Decline in Quality
Time Pressure: Studies show that when dentists work under time constraints, the quality of fillings—especially with popular bulk-fill techniques—declines significantly. Less experienced operators may perform better as they concentrate more, but routine cases are often undervalued and rushed by seasoned practitioners.
Technique Sensitivity: Modern materials like composite resins are more technique-sensitive than amalgam, requiring multiple careful steps, perfect isolation, and precise finishing. Many dentists may skip meticulous technique due to lack of time or training.
Economic and System Factors: The push for higher throughput, insurance reimbursement policies, and patient demand for rapid restoration can lead to shortcuts in execution and quality assurance.
Impact of Material Choice
Durable materials like amalgam are being replaced by esthetic composites, which demand greater skill for longevity and marginal adaptation but are less forgiving of poor technique.
Composites also require more time, careful layering, and curing, but are often placed quickly, compromising their long-term success.
Why Restoration Is Still Possible
The “lost art” can be reclaimed with a focus on preservation, careful restoration technique, and emphasizing the importance of dental craftsmanship. Quality fillings demand mindful attention to occlusion, contour, anatomical replication, and proper finishing—a practice still valued by highly skilled professionals.
A truly good dental filling is not just about closing a cavity but restoring the health, function, and appearance of the tooth—a practice endangered by modern pressures, but not extinct.
Biomimetic Restoration: Breaking the Dentin Circle of Death
These sources examine the mechanical and biological principles of tooth structure to improve modern restorative dentistry. Researchers use finite element analysis and laboratory testing to understand how stress distribution and polymerization shrinkage affect the longevity of dental repairs. A major focus is placed on the dentinoenamel junction (DEJ), a natural interface that prevents cracks from spreading and serves as a blueprint for the biomimetic approach. By utilizing immediate dentin sealing and the creation of a hybrid layer, practitioners aim to replicate this organic resilience. These advanced adhesive techniques are designed to reinforce tooth stiffness and halt the “circle of death,” a downward spiral of structural failure caused by traditional, non-bonded restorations. Ultimately, the transition toward minimally invasive procedures ensures that restorations function as a cohesive unit with the natural tooth.
The provided sources offer a comprehensive look at Biomimetic Dentistry, ranging from high-level patient education to technical scientific research on tooth structure and clinical protocols for long-lasting restorations.
1. Core Philosophy: Biomimetic vs. Traditional Dentistry
Biomimetic dentistry aims to mimic the natural properties of a tooth rather than just filling a hole or covering it with a crown.
- The “Cycle of Death”: Traditional restorative methods often lead to a cycle where a small filling eventually leads to a larger filling, then a crown, a root canal, and finally tooth loss. Biomimetic techniques aim to halt this cycle by preserving as much healthy tooth structure as possible.
- Preserving Structure: Unlike traditional crowns that require grinding down a healthy tooth to a “nub,” biomimetic restorations precisely remove only decay and cracks, then rebuild the tooth by bonding composite to healthy areas.
- Durability: Clinical studies indicate these restorations can last over 20 years while protecting against further decay and sensitivity.
2. Scientific Foundation: The Dentino-Enamel Junction (DEJ)
A significant portion of the sources is dedicated to a scientific study titled “Controlled failure mechanisms toughen the dentino-enamel junction zone”.
- The DEJ Zone: The DEJ is not a simple, weak interface but a broad functional and anatomic zone. It successfully transfers loads from the hard, brittle enamel to the more flexible dentin for a human lifetime.
- Failure Resistance: The study found that the DEJ does not undergo “catastrophic delamination”. Instead, damage is distributed over a “specialized first-formed enamel” layer approximately 40-$\mu$m wide.
- Toughening Mechanisms: The DEJ uses mechanisms like crack deflection and damage dispersion within this specialized enamel to prevent cracks from propagating into the dentin and through the entire tooth.
3. Advanced Clinical Techniques
The sources detail specific protocols used to ensure the strongest possible bond between the tooth and the restorative material.
- Immediate Dentin Sealing (IDS): This involves sealing the dentin immediately after preparation and before taking impressions. It supports delayed restoration placement and provides a reliable bond to the existing composite resin.
- Air Abrasion: This technique is used to “regain access to unreacted double bonds,” allowing for a chemical bond to the biobase. It is necessary to enhance resin-to-resin bonding in both laboratory and CAD/CAM composite restorations.
- Carious Dentin Removal: The sources emphasize using a dye containing 1% acid red propylene glycol to identify and effectively remove carious (decayed) dentin.
- Ribbond Fiber: This fiber is often used as a “cross” in the pulp chamber or as an additional layer to strengthen the foundation of the restoration.
4. Restoration Protocols
The sources provide step-by-step flowcharts for different types of restorations:
- Ceramic Restoration: Involves etching with HF (Hydrofluoric) acid (5% for 20s or 9% for 60s), ultrasonic water baths, phosphoric acid, silanization, and the application of an uncured bonding agent before seating with heated APX composite.
- Composite Restoration: Requires air abrasion (29-micron alumina), silanization, and an uncured bonding agent before seating with heated APX.
- Shrinkage Vectors: The main direction of shrinkage during polymerization is affected by the type of preparation (e.g., inlays vs. onlays). Onlays and overlays generally have stronger resistance to shrinkage vectors compared to inlays.
5. Occlusion and Functional Envelopes
The sources use animal analogies to describe how different patients’ teeth function and move:
- Rats (Normal Function): Represents a vertical envelope of function with solid maximum intercuspation (MI) controlled by the cerebellum.
- Cows (Parafunction): Represents a horizontal envelope of function, often associated with losing MI and limbic-controlled bruxism.
- Beavers (Dysfunction): Represents a front-to-back envelope of function, often seen in patients with a history of TMD (temporomandibular disorder) or Class II orthodontics.
- Fatigue Damage: Research highlights how sliding contact can cause fatigue damage in layered ceramic structures, emphasizing the need for proper occlusion management.
6. The Restoration Process (Patient View)
For a patient, the biomimetic process involves several high-tech steps:
- Diagnosis: Using magnification (loupes or microscopes) and cameras to identify decay and cracks.
- Isolation: Using a dental dam to keep the tooth clean and dry for a strong bond.
- Removal: Using cavity-detecting dye to precisely remove decay.
- Foundation: Building a “Biobase” using materials like Ribbond to seal the tooth’s nerve and protect its vitality.
- Final Restoration: Rebuilding the tooth in layers to mimic its natural strength and flexibility.