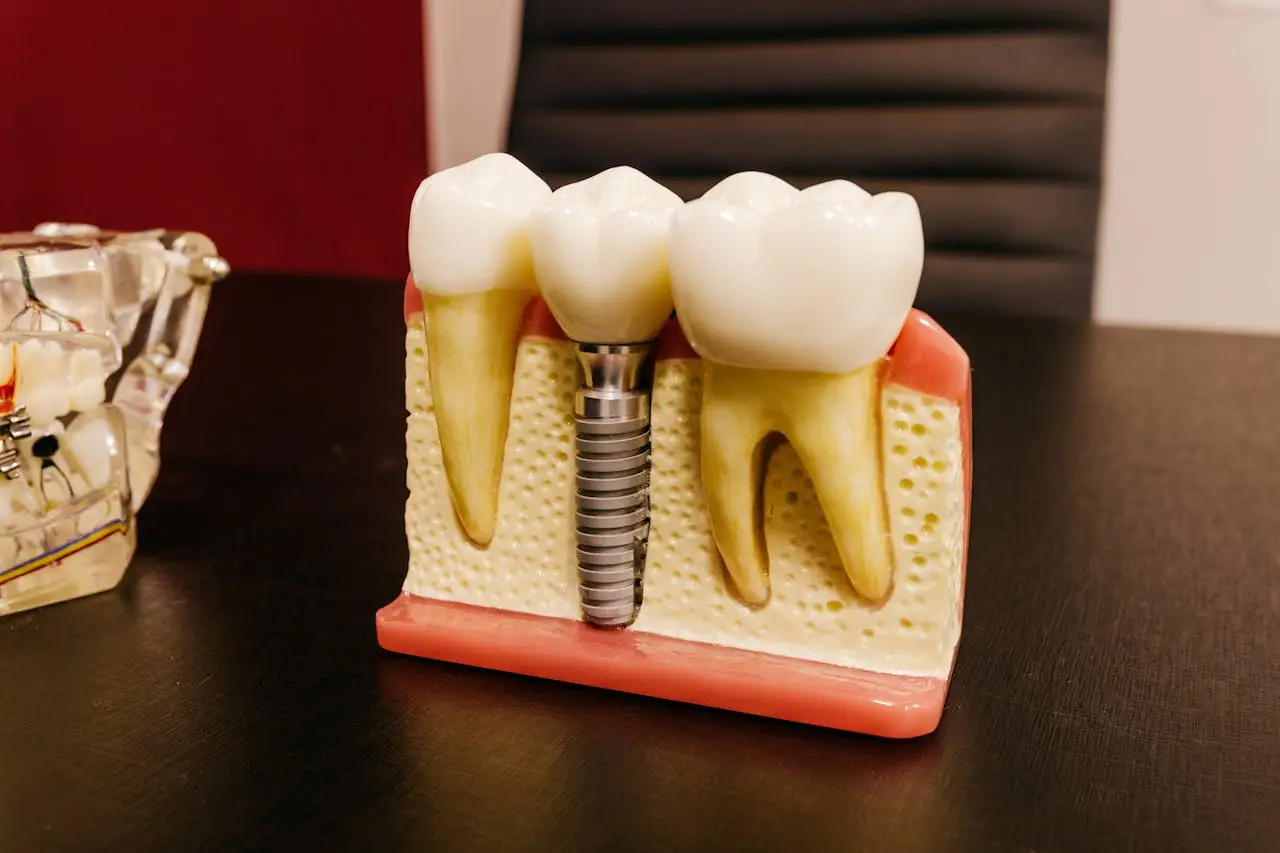
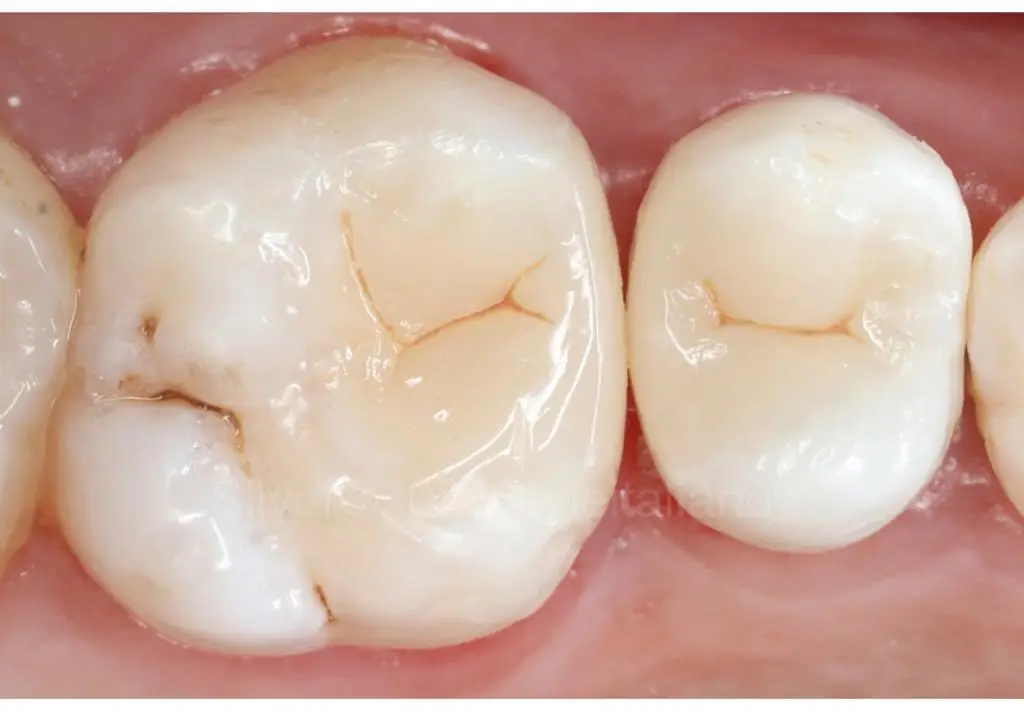
Tooth erosion is a slow, progressive thinning of enamel—the hard, protective outer layer of teeth—caused by exposure to acids rather than bacteria It is common across age groups and, if left untreated, continues toward deeper layers such as dentin and pulp, potentially leading to pain and severe dental complications
Dietary Acids:** Frequent consumption of acidic foods and drinks (soda, citrus juices, wine, pickles, vinegar) dissolves enamel. The more often and the longer these items are in contact with teeth, the greater the risk
– **Gastric Acid (Regurgitation):** Stomach acids from reflux (GERD), vomiting, eating disorders (bulimia, anorexia), or alcoholism can erode especially the back surfaces of front teeth
– **Dry Mouth & Saliva Issues:** Saliva normally protects teeth by neutralizing acids. Reduced saliva from medications, illnesses (e.g., Sjögren’s), radiation, or dehydration heightens erosion risk. Occasionally, saliva itself can be acidic enough to dissolve exposed dentin
Environmental Exposure:** Acidic fumes, workplace chemicals, or swimming in poorly maintained pools may also contribute, though such cases are rare
– **Other Factors:** Overzealous or improper brushing, some medications (like vitamin C tablets, aspirin), and genetic factors can increase susceptibility
### Signs and Symptoms
– Early: Changes in tooth color, dullness, increased sensitivity to hot/cold/sweets, surface texture changes.
– Advanced: Pain, visible yellow (dentin), pitting, chips, thinning, or transparent tooth edge
### Diagnostic Approach
Dentists recognize erosion by texture and color changes, pitting, and radiographs. They frequently ask about diet, gastric symptoms, and medical history to locate the underlying cause
### Management and Treatment
– **Early/Evolving Stages:**
– Topical fluoride (toothpaste, mouthrinse, gels, varnishes) to strengthen remaining enamel.
– Remineralizing agents as recommended by dentists.
– Gentle brushing with soft-bristled brushes; avoid brushing for at least 30 minutes after acid exposure.
– Rinse mouth with water after acidic consumption, drink through a straw if possible, and use dairy to neutralize acids- *
*Underlying Cause Management:** Address reflux, eating disorders, reduce dietary acids, or adopt saliva-promoting strategie
– **Advanced Cases:**
– Dental bonding for small areas of exposed dentin.
– Veneers or crowns for significant loss
– Professional intervention for psychological or gastrointestinal conditions.
### Prevention
– Limit acidic intake, don’t sip frequently, practice good oral hygiene.
– Regular dental visits for monitoring, early diagnosis, and intervention are crucial as enamel cannot regenerate
Early action preserves remaining enamel, prevents complications, and avoids expensive repairs in the futureTooth erosion is a progressive loss of enamel caused by acid, exposing deeper layers such as dentin and, if unchecked, the pulp. The enamel can’t regrow, so early detection and intervention are vita
### Detailed Causes
– **Diet:** Acidic foods/drinks (soda, citrus juices, wine, vinegar, pickles, energy drinks) dissolve calcium in enamel and dentin. The risk increases with frequency and time of contact
– **Gastric Acid:** Stomach acids from acid reflux/GERD, vomiting (due to eating disorders or alcoholism), or repetitive regurgitation can rapidly dissolve enamel, especially on the back of front teeth
– **Saliva Issues:** Reduced saliva (from dehydration, some medications, illnesses like Sjögren’s, or radiation) means less buffering against acids, greatly increasing erosion risk
– **Environmental Exposure:** Acidic fumes (industrial, swimming pool chlorination, battery plants) can contribute, though less common
– **Other:** Genetics, some medications (like vitamin C, aspirin), and even rare cases of naturally acidic saliva also play a role
### Effects and Progression
– **Early signs:** Dullness, sensitivity to hot/cold/sugar, color change, rough texture
– **Advanced:** Pain, yellowing (exposed dentin), pitting, chips, transparency, and ultimately decay or tooth loss
### Diagnosis and Professional Care
Dentists check for unusual wear, pitting, and color changes; they ask about dietary and medical history, possibly using dental X-rays to assess the damage.
### Specific Strategies for Management
– **Home:** Use fluoride toothpaste, rinse after acids, limit acidic intake, chew sugar-free gum, avoid brushing right after acids
– **Professional:** Topical fluoride, bonding, crowns/veneers for severe cases, treat underlying medical/dietary issues, and diagnosis of underlying health conditions if regurgitation involved
Prevention is crucial as the process is often painless initially but irreversible; regular dental visits are the best safeguard
Book an Appointment Redefine Dental Clinic Kalyan west call us today